Symptoms, diagnosis, causes, treatment and differential diagnoses of Retinitis Pigmentosa

Tunnel vision or keyhole vision is a symptom of retinitis pigmentosa
How can retinitis pigmentosa be described in a nutshell?
Retinitis pigmentosa is an inherited eye disease characterised by the progressive loss of light-sensitive cells in the retina.
This leads to a gradual deterioration of vision, often starting with night blindness and a reduced peripheral field of vision.
As the disease progresses, central visual functions may also be affected and symptoms such as reduced visual acuity, problems with colour perception and tunnel vision may occur.
What are the main symptoms of Retinitis Pigmentosa?
The main symptoms of retinitis pigmentosa include, e.g.:
- Night blindness (nyctalopia): Difficulty seeing in low light conditions, especially in the dark.
- Limited peripheral vision: Reduced perception of objects in the lateral field of vision, leading to “tunnel vision”.
- Adaptation problems to changes in light: Difficulty adapting quickly to different levels of illumination.
- Reduced visual acuity: Decrease in ability to see clear details.
- Colour recognition problems: Impaired ability to distinguish colours correctly.
- Light flash-like phenomena (photopsia): Perception of flashes of light without an external light source.
- Tunnel vision: Constriction of the visual field, only central vision remains.
- General deterioration of central vision: Decrease in central visual acuity over time.
What are the possibilities of diagnosing Retinitis Pigmentosa?
These diagnostic methods provide an accurate assessment of retinitis pigmentosa and are essential for developing an individualised treatment plan:
- Basic eye examination: Includes vision tests, slit lamp examination and ophthalmoscopy to detect changes in the retina.
- Visual field test: Checks the peripheral field of vision for limitations that may occur with RP.
- Electroretinogram (ERG): Measures the electrical activity of the retinal cells to identify abnormalities.
- Optical Coherence Tomography (OCT): Provides detailed images of the retinal layers to visualise structural changes.
- Genetic testing: Identify genetic mutations associated with RP to confirm diagnosis.
- Dark adaptation test: Measures the eyes’ ability to adapt to darkness, which may be impaired in RP.
- Fluorescein angiography: Uses coloured contrast media to monitor blood flow and fluid build-up in the retina.
What causes are associated with the diagnosis of Retinitis Pigmentosa?
Retinitis Pigmentosa is mainly caused by genetic factors, and different inheritance patterns can influence the development of this retinal disease:
- Genetic mutations: Most often, retinitis pigmentosa is caused by mutations in various genes that are important for retinal cell function and the visual process.
- Autosomal recessive inheritance: A large proportion of cases follow an autosomal recessive pattern of inheritance, where both parents must carry the defective gene in order to pass the disease to the child.
- Autosomal-dominant inheritance: In some cases, the disease can also be inherited in an autosomal-dominant manner, where only one copy of the defective gene from one parent is sufficient to cause the disease.
- X-linked inheritance: Rarely, retinitis pigmentosa is transmitted by X-linked inheritance, with males being more susceptible due to their single X chromosome.
What options are there for Retinitis Pigmentosa treatment?
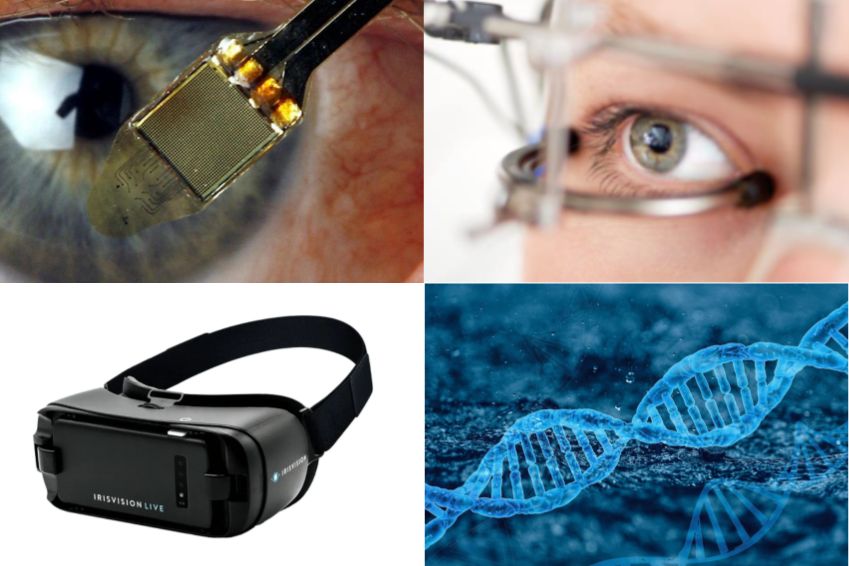
Retinitis pigmentosa treatment includes innovative approaches such as retinal implants, transcorneal electrostimulation, gene therapy and proven methods such as optical and electronic visual aids.
In addition, the treatment of concomitant diseases as well as complementary approaches and a targeted diet play a decisive role.
- Retinal implants: Advanced technology for the partial restoration of vision in retinitis pigmentosa. An electronic device replaces defective photoreceptors by placing electrodes on the retina.
- Transcorneal electrical stimulation (TES): Stimulates remaining retinal cells through electrical impulses on the cornea. Outpatient treatment without invasive surgery with promising results but varying degrees of effectiveness.
- Gene therapy: Corrects or replaces defective genes that cause retinitis pigmentosa. By injecting healthy genes with the help of viruses, promising but still experimental and subject to further research.
- Optical aids and visual aids: Glasses, magnifiers and adaptations improve existing vision. Customised solutions promote independence and extend the peripheral field of vision.
- Electronic visual aids: Utilises technology such as wearable cameras for audible or tactile signals. Facilitate orientation and the recognition of obstacles despite progressive vision loss.
- Treatment of concomitant diseases: Cataracts can be improved by surgery and clear intraocular lenses. Anti-inflammatory medication or injections help with macular oedema.
- Complementary methods: Homeopathy, nutrition and herbal supplements support well-being.
- Nutrition and dietary supplements: A balanced diet with antioxidants, omega-3 fatty acids and vitamins. Nutritional supplements such as vitamin A, vitamin E to support retinal health.
What are the most important differential diagnoses for Retinitis Pigmentosa?
The exact identification of Retinitis Pigmentosa requires a differentiated approach, as different eye diseases can have similar symptoms.
Five important differential diagnoses are briefly outlined here to illustrate the challenges involved in making a precise diagnosis.
- Usher syndrome: Genetic disease with simultaneous occurrence of progressive deafness and Retinitis Pigmentosa; different types, type I most severe form.
- Choroideremia: Rare genetic disease with specific loss of choroidal cells, in contrast to Retinitis Pigmentosa.
- Leber congenital amaurosis (LCA): Rare genetic disease, affects several organ systems in addition to the retina; manifests itself in early childhood.
- Cone dystrophy: Loss of cone cells leads to predominantly central visual loss, while peripheral visual functions can be preserved for longer.
- Cone-Rod dystrophy: Simultaneous loss of cone and rod cells, resulting in combined impairment of central and peripheral vision; colour discrimination is particularly affected.